blog
Vascular Occlusion in Dermal Filler Treatments – What Injectors Must Know to Stay Safe

Aug 18 2025
Reading Time: 5 Minutes
Author:
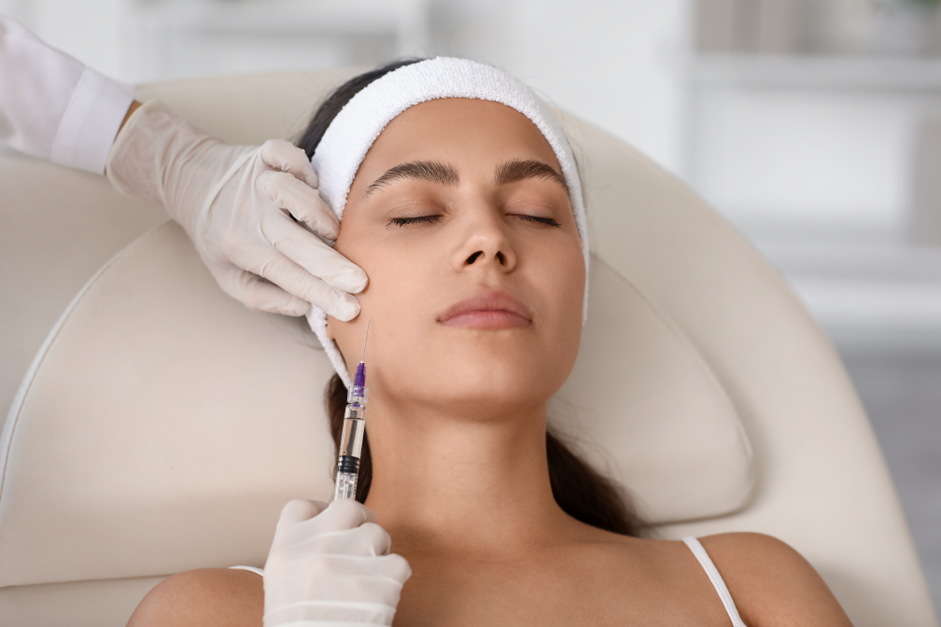
Dermal fillers are now very popular in medical spas and cosmetic clinics. They restore volume, sculpt features, and smooth wrinkles. They also require little to no downtime. But injections into the face carry risks.
A serious complication is vascular occlusion. It is rare but a true medical emergency. Every injector must recognize and manage it immediately. Quick action prevents tissue necrosis, scarring, or blindness.
This guide covers what you need to know about vascular occlusion. It is for new nurses and experienced injectors alike. Understanding this complication is about patient safety and professional responsibility.
All images used under license from Canva. © APT Medical Aesthetics, 2025. All rights reserved.
What Is Vascular Occlusion
A vascular occlusion happens when filler enters an artery or compresses it. This blocks blood flow to nearby tissues. Facial arteries supply the nose, lips, and eyes. Compromised blood flow can have devastating effects.
Occlusion can be intravascular or extravascular. Intravascular means filler is injected directly into an artery. This is more dangerous. Extravascular means product compresses a vessel from outside. Symptoms are similar but damage is usually less severe.
Worst outcomes include skin death, disfigurement, and permanent vision loss. Learning to prevent, identify, and treat this is critical for every injector.
All images used under license from Canva. © APT Medical Aesthetics, 2025. All rights reserved.
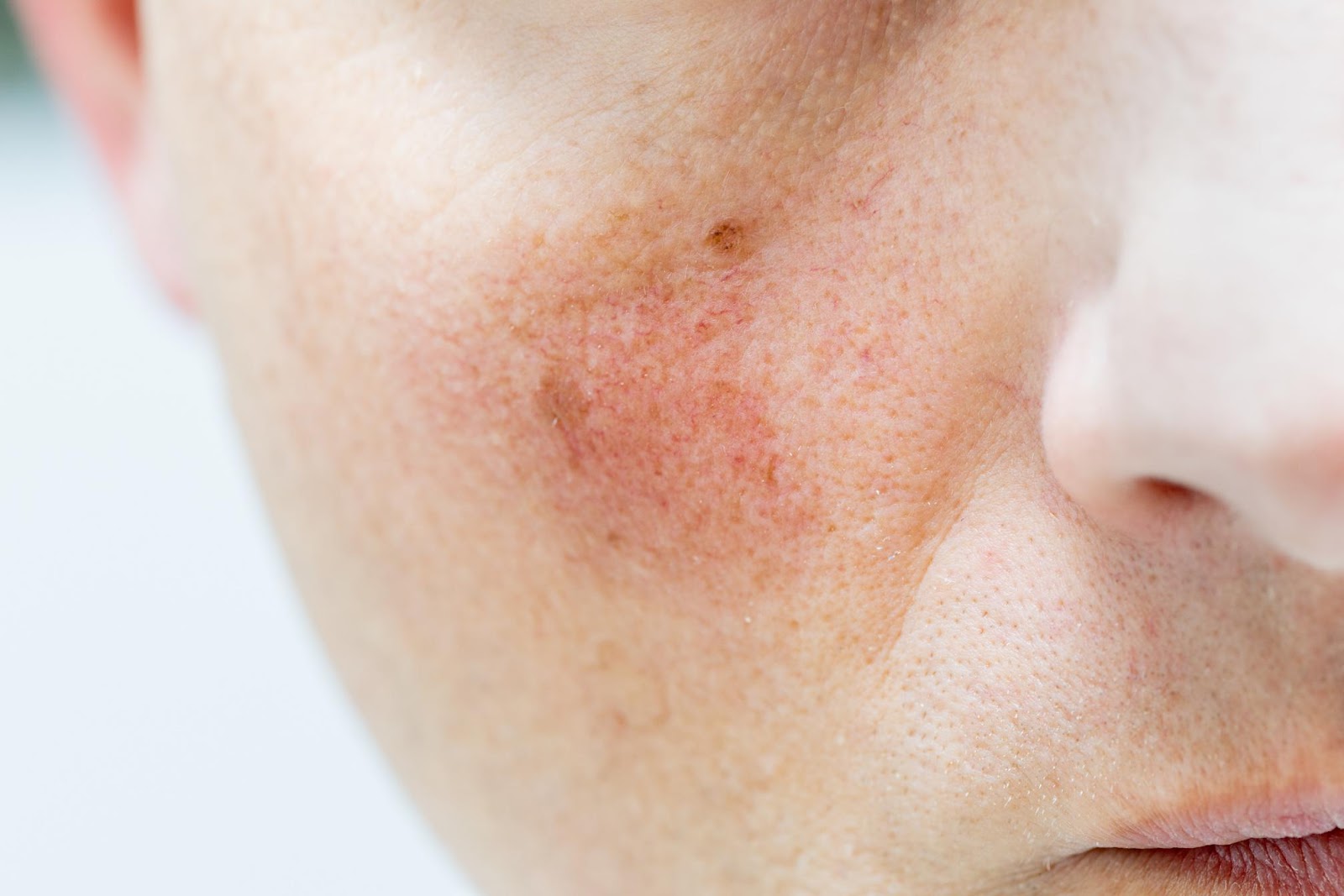
Recognizing the Signs of Vascular Occlusion
Early recognition gives the best chance to reverse damage. Signs appear immediately or within minutes. You must spot subtle changes and respond without delay.
Key warning signs include
- Severe, sudden pain during or after injection
- Skin blanching (whiteness or paleness in a specific area)
- Livedo reticularis (a mottled, web-like pattern on the skin)
- Coolness or decreased temperature of the affected area
- Dusky, grey, or purplish skin color
- Delayed capillary refill
- Progressive discoloration or breakdown of skin tissue
If the area is painful or shows vascular changes, treat it as a potential occlusion until proven otherwise.
High-Risk Areas for Vascular Occlusion
Some face areas are more prone to occlusion. Their vascular anatomy and limited collateral circulation increase risk. Treat these zones with extra caution and precise technique.
All images used under license from Canva. © APT Medical Aesthetics, 2025. All rights reserved.
High-risk injection sites include
- Nasolabial folds
- Glabella (area between the eyebrows)
- Nose
- Lips
- Tear troughs (under-eye hollows)
- Forehead and temple
- Chin and jawline
These areas have arteries like the angular, supratrochlear, and dorsal nasal. Improper depth, angle, or pressure can compromise vessels.
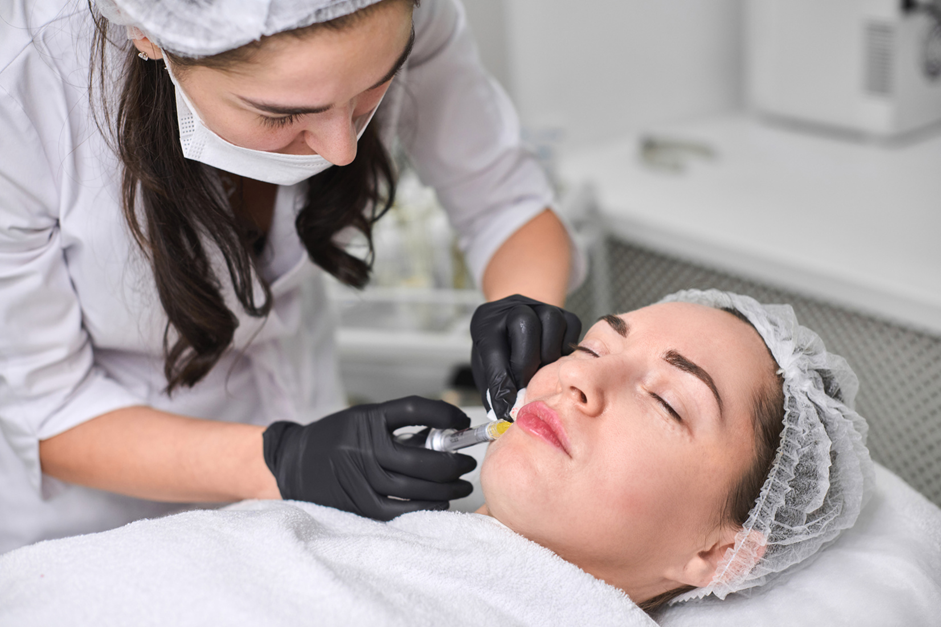
Prevention Starts With Proper Training
Complications can happen to anyone. But proper education and technique lower the risk of occlusion. Good injection courses for nurses focus on facial anatomy, safety, and complication management.
Here are essential safety principles from high-quality training programs
- Always aspirate before injecting to check for blood return
- Inject slowly with minimal pressure
- Use small aliquots rather than large boluses
- Understand the depth and plane for each area
- Know the location and course of facial arteries
- Consider using a cannula in high-risk zones
- Be ready with emergency protocols and reversal agents
All images used under license from Canva. © APT Medical Aesthetics, 2025. All rights reserved.
Training teaches you where to inject and when not to. It also covers how to react under pressure. This protects your patients at every step.
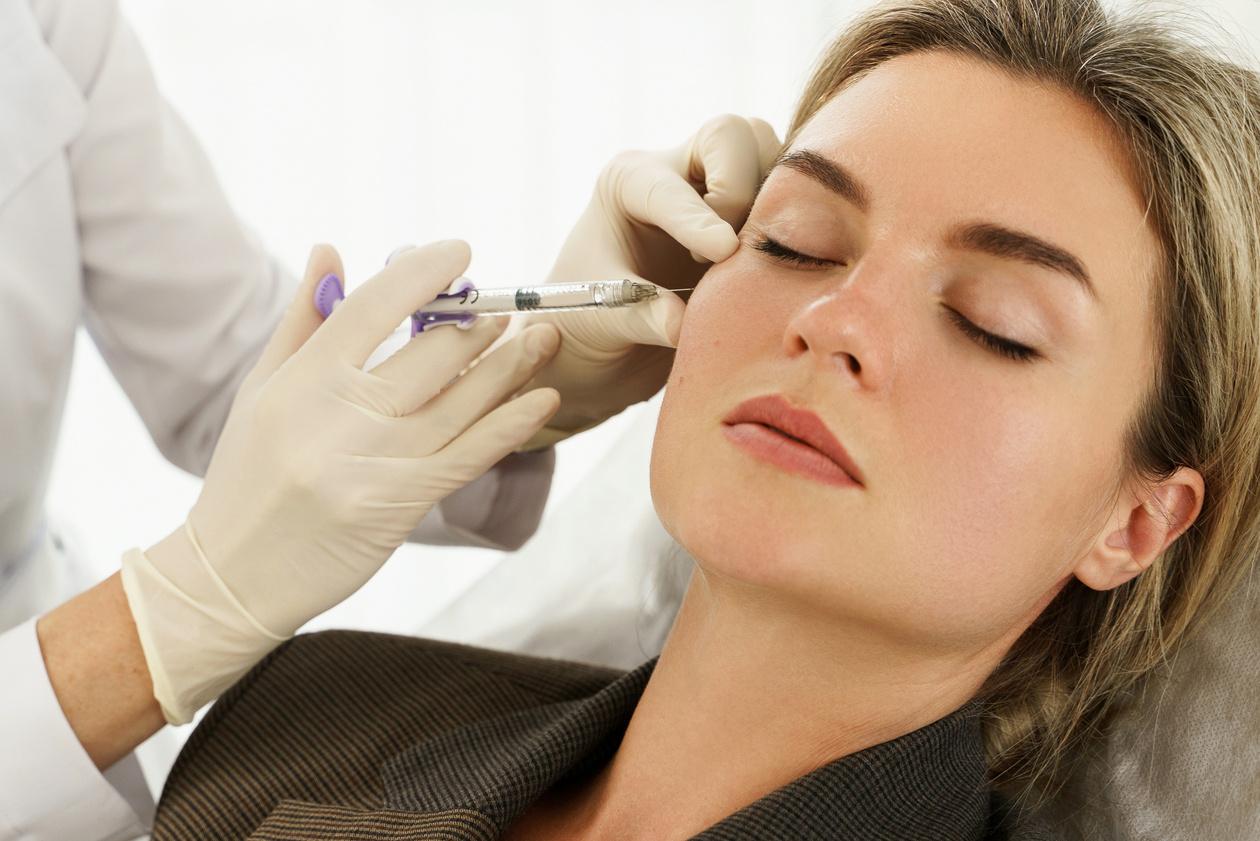
Using a Cannula to Improve Safety
A cannula is a blunt-tipped, flexible tool. It distributes filler through one entry point. Its blunt tip is less likely to pierce a blood vessel. This makes it safer for high-risk areas.

All images used under license from Canva. © APT Medical Aesthetics, 2025. All rights reserved.
Cannulas come in different lengths and gauges. They need a specific insertion technique. They are especially useful for
- Cheeks
- Tear troughs
- Nasolabial folds
- Jawline contouring
- Marionette lines
Cannulas are not risk-free but are a valuable safety tool. Proper training is needed before switching from needles. The technique and feel are different.
Emergency Protocols for Vascular Occlusion
Knowing how to identify occlusion is only part of the solution. A clear, practiced emergency protocol protects patients. All injectors must act immediately when occlusion is suspected.
Standard treatment for vascular occlusion involves
1. Stop the Injection Immediately
Cease injecting at the first sign of pain, blanching, or vascular changes
2. Massage the Area Gently
Sometimes gentle massage relieves external compression. Be careful not to spread the filler.
3. Apply Warm Compresses
Warming the area can improve blood flow and tissue oxygenation.
4. Administer Hyaluronidase if Using Hyaluronic Acid Filler
This enzyme breaks down hyaluronic acid. It reverses the filler and relieves the blockage.
5. Contact a Medical Director or Physician Immediately
Even experienced injectors need collaboration during emergencies.
6. Monitor the Patient Closely
Follow up regularly to check for delayed tissue compromise.
7. Refer to a Specialist if Vision Is Affected
Any visual symptoms need urgent referral to an ophthalmologist or ER.
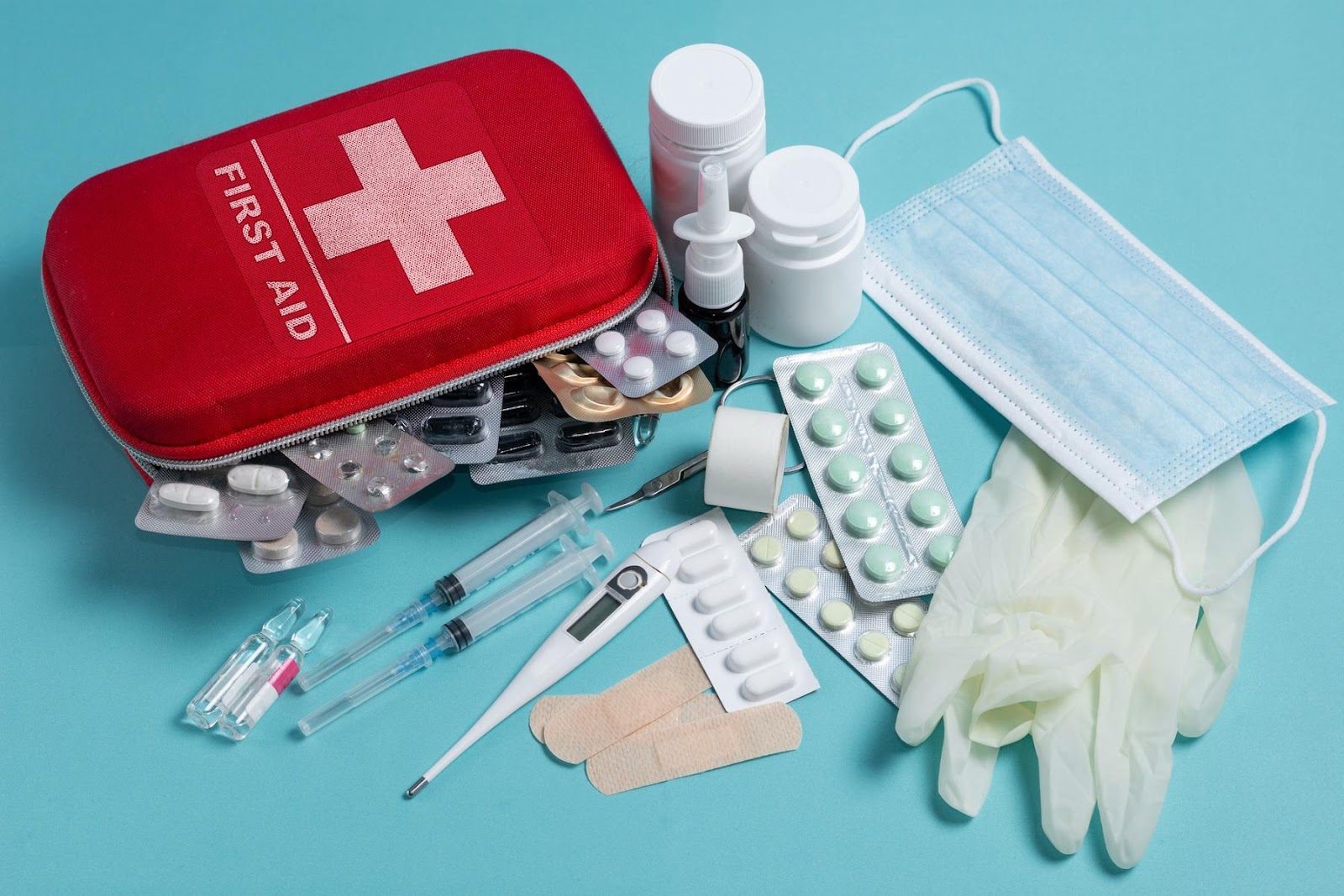
Every injector should have a vascular occlusion emergency kit. It should include hyaluronidase, syringes, sterile saline, gloves, alcohol swabs, and written protocols. Practice your response regularly to act decisively.
Why Complication Management Belongs in Every Training Program
Not all training courses focus on vascular safety. Many fast-track or online programs skip real-world complications. This leaves new injectors unprepared for clinical practice.

All images used under license from Canva. © APT Medical Aesthetics, 2025. All rights reserved.
Choose programs with comprehensive facial anatomy and emergency training. You should know how to inject and how to protect patients. At APT Injection Training, our courses for nurses meet high safety standards. We focus on hands-on learning, anatomy, and complication response.
The Legal and Ethical Responsibility of Safe Injection
As a regulated healthcare professional, you must uphold high patient care standards. Injecting fillers is a controlled act. It requires caution, skill, and preparation. Ignorance is not an excuse for complications.
Maintain liability insurance and follow professional guidelines. Work under a medical directive if you are not a prescriber. Collaborating with a medical director provides oversight and support for
Tips to be a
Successful Injector!
Free E-Book download
 Student Log in
Student Log in
 1267 Cornwall Rd, Unit 300, Oakville, Ontario L6J 7T5
1267 Cornwall Rd, Unit 300, Oakville, Ontario L6J 7T5

 (289) 271-5718
(289) 271-5718